Clinical Rotations
Clinical training takes place primarily at the new, state-of-the-art Van Ness Campus (video tour) of CPMC (opened 3/2019) that is a tertiary referral center for Sutter Health as well as for Northern California, providing advanced cardiac care including complex coronary intervention, structural heart intervention, cardiac electrophysiology, and advanced heart failure and heart transplantation. All acute cardiac services were moved from the Pacific Campus of CPMC, the site of the original Cooper Medical College (established 1890) and Stanford University School of Medicine (1909-1959). Two months are also spent at the new Mission Bernal Campus (video tour) of CPMC (opened 8/2018) in the Mission district of San Francisco that serves an underserved patient population as well as houses the Acute Care for the Elderly (ACE) unit for older adults. This new campus was built to replace St. Luke’s Hospital (established 1871), one of the original hospitals in San Francisco.
Our 9 cardiology fellows (3 per year) are integral members of the cardiovascular services and laboratories, and work side-by-side with core faculty and attending cardiologists in every aspect of the cardiovascular division. All fellows also participate in monthly institutional cardiovascular process improvement meetings as members of specific workgroups. While gaining exceptional clinical training, fellows also take an active role in supervising and teaching interns and residents from the CPMC Internal Medicine Residency program, as well as medical students from Geisel School of Medicine at Dartmouth and UCSF.
Clinical rotations are distributed over 3 years with core rotations (required by ACGME/COCATS) concentrated in the first two years. This allows for more time in Year 3 to customize training using months reserved for elective rotations, whether it be for advanced fellowships preparation, advanced COCATS achievements, or other specific career goals. The more condensed rotation schedule during the first year also allows full exposure to the breath of cardiology so that fellows can make a decision for sub-specialization early.
| ROTATION | YEAR 1 | YEAR 2 | YEAR 3 |
|---|---|---|---|
| Consultative Cardiology | 2 | 1 | 1 |
| Mission Bernal Campus Cardiology | 1 | 1 | |
| CCU / Telemetry Service | 1 | 2 | 1 |
| Advanced Heart Failure / Transplant Service | 1 | 1 | |
| Electrophysiology Service | 1 | 1 | |
| Cardiac Catheterization Laboratory | 2 | 1 | 1 |
| Echocardiography Laboratory | 2 | 2 | |
| Noninvasive Cardiology Laboratory | * | * | * |
| Nuclear Cardiology Laboratory | 1 | 1 | |
| Structural Heart / Cardiac Surgery | 1 | 1 | |
| Advanced Cardiac Imaging | 2 | ||
| Adult Congenital Heart Disease | ** | ** | ** |
| Ambulatory Cardiology | *** | *** | *** |
| Elective / Research | 1 | 1 | 6 |
| Total (Months) | 12 | 12 | 12 |
* Biweekly coverage schedule throughout year
** Dedicated curriculum during Echocardiography rotation
*** Weekly ½ day at assigned office throughout year
Consultative Cardiology

The cardiology inpatient consult rotation represents the foundation of clinical training at this program that aims to train exceptional clinical cardiologists. As a tertiary referral center for the Sutter Health system and for all of Northern California, CPMC receives the most complex referrals and transfers, and fellows on the consult rotation have a high-quality consultative experience. The fellow works directly with the attending cardiologists assigned to the inpatient service for the week, and together with the attendings, manages a wide array of clinical pathologies on the general medicine and surgical wards, on the obstetrics floor, and in the intensive care units. Common consultation topics including management of acute coronary syndrome, arrhythmias, heart failure, pre-operative cardiac evaluations, and post-operative cardiac management. Consult service census ranges from 10-20 patients per day.
Mission Bernal Campus Cardiology

Two months are dedicated to managing the cardiology service at the Mission Bernal Campus of CPMC. This campus is located 12 minutes directly south of the Van Ness Campus in the Mission and Bernal Heights districts of San Francisco and serves a more underserved patient population. Consequently, clinical pathologies such as rheumatic heart disease, infectious endocarditis, and peripartum cardiomyopathy are seen at higher frequency during this rotation. The fellow provides direct cardiology consultative services and coordinates patient care with the emergency department and hospitalist services as the primary cardiologist. Daily rounds take place with the faculty cardiologist to discuss management decisions. The fellow also runs the weekly discharge clinic where patients are seen following discharge from the hospital for continuity of care.
Coronary Care Unit / Telemetry Service

There are two inpatient cardiology teams that make up the cardiology service at the Van Ness Campus of CPMC. Each team is staffed by one of the two cardiology practices, Sutter Foundation Cardiology and Golden Gate Cardiology, and has a dedicated internal medicine resident, intern and medical students. Critical cardiac patients are cared for in any of the beds in the open ICU that make up the entire 6th floor of the medical center. All other cardiac patients are cared for in any of the private rooms on the 9th and 10th floors that are enabled for telemetry monitoring and staffed with specialized cardiac nursing. The fellow on this rotation functions as a junior attending, and supervises both teams, coordinating work rounds with the weekly attending from each group, and coordinating patient care with other services such as advanced heart failure, interventional and structural heart, electrophysiology, cardiothoracic surgery, and advanced cardiac imaging. The fellow is also responsible for housestaff and student teaching.
Advanced Heart Failure / Transplant Service
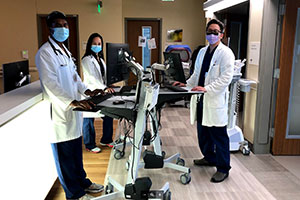
Because of the wealth of clinical experience on this service, and at the request of fellows, the program has extended the heart failure rotation from 2 months (required by COCATS) to 4 months. There has been a long history of cardiac transplantation and LVAD innovation at this institution, and the Center for Advanced Heart Failure Therapies and Transplants at CPMC continues to be one of the highest volume services at CPMC, drawing referrals and transfers of end-stage heart failure and acute cardiogenic shock from Sutter Health hospitals throughout the region. The fellow is an active member on a multidisciplinary team that includes advanced heart failure cardiology, transplant surgery, structural heart, critical care, and the in-house NP team. While on service, the fellow is responsible for a dedicated list of patients, drives discussions on these patients during rounds, and directly manages care with the nurse practitioners. Fellows gain experience in the entire spectrum of mechanically-assisted circulatory support, including IABP, Impella and ECMO, as well as gain exposure to postoperative LVAD and transplant care. Fellows also participate in selection committees for LVAD and heart transplantation.
Electrophysiology Service
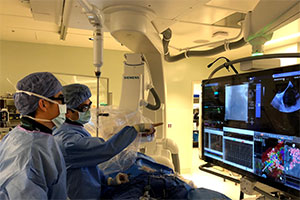
Fellows experience arrhythmia management throughout their clinical training, participating in the evaluation and treatment of atrial fibrillation, heart block, SVT, VT, cardiac arrest, as well as pacemaker and ICD management. The Electrophysiology Service rotation provides a more intensive experience in advanced cardiac electrophysiology, managing the inpatient EP service as well as participating in the EP laboratory. The Atrial Fibrillation and Complex Arrhythmia Center at CPMC is a referral center for high-acuity and high-complexity cases from across Northern California. Fellows are able to experience the entire range of EP studies, complex catheter-based interventions including epicardial ventricular tachycardia ablations, as well as pacemaker and ICD implantation and extractions. There are no electrophysiology subspecialty fellows, allowing cardiology fellows to gain unrivaled experience in the EP laboratory. For fellows interested in advancing to electrophysiology fellowship, case volume and hands-on involvement in specialized laboratory skills such as coronary sinus cannulation and transseptal puncture have been advantageous attributes. Even if fellows are not planning to pursue an electrophysiology fellowship, the program offers COCATS Level II achievement with optional training in pacemaker implantation (this will require dedicating another 4 months of elective time to pacemaker and ICD management and implantation).
Cardiac Catheterization Laboratory
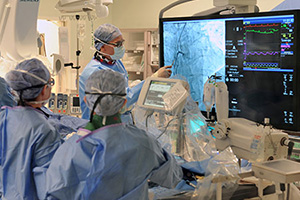
Four dedicated months allow for concentrated time in the cardiac catheterization laboratory to gain proficiency in right and left heart catheterization, hemodynamic interpretation, coronary angiography and valvular assessment. There are no interventional cardiology subspecialty fellows, allowing cardiology fellows to be first-assist in virtually any case. For fellows interested in advancing to interventional and structural fellowship, case volume and hands-on involvement, not only in coronary interventions, but also in structural heart cases have been advantages during the subspecialty fellowship application process. Additional experience in the catheterization laboratory is gained during the Structural Heart rotation (see below). Due to the high volume of catheterization laboratory cases at the Van Ness Campus at CPMC, most fellows, even if they are not planning to pursue additional fellowship training in interventional cardiology, will achieve COCATS Level II that will allow them to perform procedures in the catheterization laboratory once they are in practice.
Echocardiography Laboratory

Four dedicated months in the echocardiography laboratory allow fellows to master skills in performing and interpreting transthoracic and transesophageal echocardiography, and gain proficiency in managing adult congenital heart disease. Fellows average 15-20 transthoracic interpretations per day and perform 3-5 transesophageal echocardiograms per day. Fellows attend a ½ day adult congenital heart disease clinic that manages a large population of patients with congenital heart disease cared for at CPMC for over 50 years. Fellows actively participate in the management of a wide variety of conditions including ASD, VSD, Tetralogy of Fallot, and partial anomalous pulmonary venous return. CPMC is an active center of the Bay Area Adult Congenital Society, and our fellows present cases at the society conference biennially. With the high-volume of cases, all fellows easily achieve COCATS Level II in echocardiography, and develop a thorough understanding of physiologic and hemodynamic principles of transthoracic, transesophageal, contrast, 3-dimensional, and speckled tracking strain echocardiography. During rotations in the cardiac catheterization and EP laboratories, fellows also gain experience in intracardiac echocardiography. For fellows interested in advanced echocardiography training, there is a curriculum that includes experience in intraprocedural and intraoperative transesophageal echocardiography during structural intervention and cardiac surgery, and fellows are able to achieve COCATS Level III by dedicating an additional 3-6 months of elective time to advanced echocardiography.
Non-Invasive Cardiology Laboratory

Fellows get comprehensive exposure to the non-invasive cardiology laboratory at the Van Ness Campus and are trained to become proficient in supervising and reading the full spectrum of non-invasive testing such as Holter monitoring, event monitoring, treadmill stress testing, and tilt-table testing.
Nuclear Cardiology Laboratory / Advanced Cardiac Imaging

During the dedicated nuclear cardiology rotation, fellows gain concentrated experience in the operations of the nuclear cardiology laboratory, and also have dedicated time for in-depth nuclear study reading. During the advanced cardiac imaging rotation, fellows spend structured time with our advanced cardiac imaging radiologist and read nuclear studies, structural CTs, coronary CTs, coronary calcium scans and cardiac MRIs. As a referral center for advanced cardiomyopathies, patients are routinely transferred to CPMC for evaluation and management of conditions such as cardiac amyloidosis, cardiac sarcoidosis, and arrhythmogenic right ventricular cardiomyopathy, and fellows receive training in nuclear cardiology and cardiac imaging year round while on other rotations such as consultative cardiology, CCU and advanced heart failure. The multidisciplinary conferences are attended by cardiac radiology, and detailed and high-level discussions ensue among fellows and faculty while viewing and interpreting high-definition images on the conference room projector screen.
Structural Heart / Cardiac Surgery
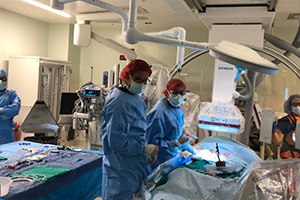
The newly redesigned structural heart and cardiovascular surgery rotation provides a dedicated month during each of the second and third years of a cutting-edge experience in valvular disease management. In this new era of transcatheter valvular therapeutics, cardiologists finishing training must be proficient in understanding and applying the newest concepts and therapies available. Bay Area Structural Heart at CPMC is a premier structural heart program that is involved in multiple clinical trials and has access to procedures and devices that place the program truly at the leading edge of this rapidly evolving field. Fellows are able to participate in transcatheter cases including TAVR, TMVR, TTVR, MitraClip, ASD closure, and WATCHMAN left atrial appendage closure, and assist with intraprocedural transesophageal structural imaging.
Adult Congenital Heart Disease

Care of adult patients with congenital heart disease occurs over multiple rotations. In addition to providing direct patient care, there is a yearlong lecture series given by Stanford Adult Congenital Heart specialists. Our weekly adult congenital heart clinic, run in conjunction with other local Adult Congenital specialists, allows fellows to manage a wide variety of disorders. There is robust participation in the Bay Area Adult Congenital Society with biannual case presentations by the fellows.
Ambulatory Cardiology

The ambulatory cardiology curriculum involves fellows managing a panel of patients directly in the offices of the core faculty. Each year, each fellow is assigned to a faculty cardiologist, and will go to their office ½ a day per week to see new outpatient consultations and see these patients in follow-up throughout that year. Patients are typically seen by the fellows first, then are seen with the fellow and the attending physician together. By being in an actual cardiology office setting, fellows also learn to interact and work with office staff and other clinical providers such as medical translators, nurses, nurse practitioners, and physician assistants. The yearly assignment process starts with the fellow submitting their choices of offices. With available subspecialty faculty, fellows are able to gain deeper experience in subspecialties within cardiology if interested, such as in interventional cardiology, structural heart disease, electrophysiology, or advanced heart failure. With different offices to choose from, fellows can also be exposed to different practice models, ranging from smaller private, to foundation, to university-affiliated practices. This in-depth exposure to the workings of cardiology offices has provided fellows important insight during the job search process.
Elective / Research

During semiannual performance evaluation sessions with the program director, fellows will actively discuss and plan how to utilize elective months. For each elective month, a rotation objective with specific learning goals will be submitted to the program director for approval. Electives are utilized according to the training objectives of each fellow, and may include time directed toward achievements of COCATS Level II in cath lab, EP lab, pacemaker implantation, vascular medicine, nuclear cardiology, cardiac CT, cardiac MR, or COCATS Level III in echocardiography. Electives can also be structured for research, preparation for advanced fellowship, rotations at outside institutions, and for other specific career goals.
Living in San Francisco
There’s never a dull moment in San Francisco, a national hub for culture, dining, outdoor activities, local events, theater and parades. Experience the mountains, beach, and city in one iconic place that’s an easy drive away from wine country or skiing.
Contact Us
Program Coordinator
Wanda Keith
415-600-5966
415-447-6322 fax
wanda.keith@sutterhealth.org
Associate Program Director
Andrew Rosenblatt, MD, FACC
Program Director
Richard H. Hongo, MD, FACC, FHRS




